Ocular
Oculoplastics and the Orbit
Ocular signs can reveal systemic disease. Clare Quigley MD reports from Kilkenny, Ireland.

Clare Quigley
Published: Tuesday, July 19, 2022
The important systemic associations of ocular pathology featured in the European Society of Ophthalmology honorary lecture delivered by Dr Elizabeth McElnea at the Irish College of Ophthalmologists annual conference.
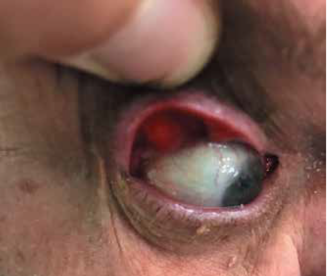
She began by presenting the case of an overweight 35-year-old man who presented with a corneal abrasion and a complaint of discharge from both eyes each morning. The patient had diffuse punctate corneal epithelial defects and easy eyelid eversion in keeping with Floppy Eyelid Syndrome (FES). Dr McElnea discussed anterior segment complications encountered in FES, including corneal ulceration - which may progress to descemetocele formation and frank perforation - and posterior segment associations, including non-arteritic anterior ischaemic optic neuropathy. She moved on to the main systemic association of FES that carries an increased risk of mortality for the patient.
“The association of floppy eyelid syndrome with obstructive sleep apnoea is so strong that, with discovery of the former, a sleep study should be considered. While nearly all floppy eyelid syndrome patients have obstructive sleep apnoea, not all patients with obstructive sleep apnoea have floppy eyelid syndrome. Those that do however tend to be younger and more obese, with higher indices of severity of sleep apnoea,” she noted.
Onward referral for a polysomnogram, or sleep study, is required for diagnosing sleep apnoea. Once confirmed, management techniques such as weight loss and continuous positive airways pressure (CPAP) can reduce associated morbidity and mortality. Approaches differ for managing the lids in FES. The surgeries adopted for floppy eyelid syndrome tend to be variations of upper lid wedge resections and tarsal strips, she explained.
Among the other cases discussed, Dr McElnea included a pair of patients with bilateral ptosis with poor levator function. These patients were found to have reduced ocular movements, cataract, and corneal decompensation in addition to their droopy upper eyelids, with the possibility of systemic myopathy acknowledged. Muscle biopsy yielded an important finding: cytochrome oxidase (COX)-negative fibres, indicating mitochondrial cytopathy. Ophthalmologists know mitochondrial disorders to cause ocular movement disorders such as Chronic Progressive External Ophthalmoplegia (CPEO) and optic neuropathy such as Leber Hereditary Optic Neuropathy (LHON), but corneal complications in mitochondrial pathology are less well known.
“Corneal endothelial cells maintain corneal stromal deturgescence and have large numbers of mitochondria to support the high metabolic activity that this function demands. Despite this, corneal endothelial involvement in mitochondrial disease is not typical and, to date, only sporadically reported. In the cases described the diagnosis of a mitochondrial disorder could account for all the patients” clinical features—ophthalmoplegia, corneal endothelial dystrophy, cataract, and, in the first case, sensorineural deafness. Ophthalmologists should consequently be cognisant of the possibility of corneal endothelial involvement in mitochondrial disease,” she advised.
Elizabeth McElnea is a Consultant Ophthalmic and Oculoplastic Surgeon at University Hospital Galway, Ireland.
Latest Articles
Towards a Unified IOL Classification
The new IOL functional classification needs a strong and unified effort from surgeons, societies, and industry.
The 5 Ws of Post-Presbyopic IOL Enhancement
Fine-tuning refractive outcomes to meet patient expectations.
AI Shows Promise for Meibography Grading
Study demonstrates accuracy in detecting abnormalities and subtle changes in meibomian glands.
Are There Differences Between Male and Female Eyes?
TOGA Session panel underlined the need for more studies on gender differences.
Simulating Laser Vision Correction Outcomes
Individualised planning models could reduce ectasia risk and improve outcomes.
Need to Know: Aberrations, Aberrometry, and Aberropia
Understanding the nomenclature and techniques.
When Is It Time to Remove a Phakic IOL?
Close monitoring of endothelial cell loss in phakic IOL patients and timely explantation may avoid surgical complications.
Delivering Uncompromising Cataract Care
Expert panel considers tips and tricks for cataracts and compromised corneas.
Organising for Success
Professional and personal goals drive practice ownership and operational choices.