Innovation in Visualisation During Vitreoretinal Surgery
Benefits of new digitally enabled microscope-integrated intraoperative OCT surgical platform.

Cheryl Guttman Krader
Published: Friday, September 30, 2022
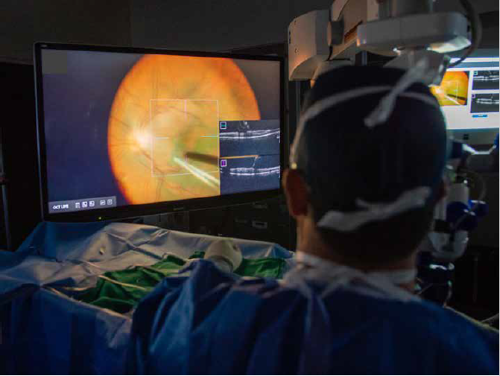
A digitally enabled high definition, heads-up stereoscopic intraoperative OCT system could help surgeons overcome their fondness for the flatscreen.
The DISCOVER (Determination of feasibility of Intraoperative Spectral domain microscope Combined/integrated OCT Visualization during En face Retinal and ophthalmic surgery) study found surgeons liked the idea of intraoperative OCT (iOCT) for vitreoretinal procedures for both conventional microscope-integrated and digitally enabled platforms. However, they often preferred to use the large, screen- and surgical field-based visualisation of the iOCT data stream.
“Intraoperative OCT is an exciting innovation in vitreoretinal surgery—and previously we showed in the prospective DISCOVER study that it was feasible and useful. However, the study also found surgeons strongly preferred visualising the OCT data on a 2D screen that required looking away from the surgical field compared to using the OCT data injected into the microscope oculars. Therefore, we felt there was a need for a new integrative surgical theatre integrating intraoperative OCT with a 3D heads-up display,” explained Katherine Talcott MD.
INTEGRATIVE TECHNOLOGIES
“A digitally enabled option for high-definition, heads-up stereoscopic intraoperative visualisation is now available, giving an immersive 3D visualisation of both the surgical field and the iOCT data stream. Our study indicates this technology allows for greater surgical visualisation efficiency, as well as other advantages. Additional studies are now needed to better assess patient outcomes, surgeon experience, and overall value of integrative technologies designed to enhance the surgical theatre experience.”
The DISCOVER study is an IRB-approved multi-surgeon case series. Comparative assessment of surgical visualisation efficiency (i.e., the proportion of cases performed with the ocular headsup display in the conventional group or the 3D screen-based visualisation in the digitally enabled group versus cases with the external 2D monitor for each system) was the primary objective of the post-hoc analysis. It included 100 cases performed using a conventional microscope-integrated iOCT (Rescan 700, Zeiss) and 100 with the digitally enabled iOCT (Artevo 800, Zeiss).
“The Artevo 800 is described as the first 3D-capable digital ophthalmic microscopic. It features a hybrid mode that allows the surgeon to view the surgical field using a 55-inch 4K resolution monitor or through the oculars, and it may offer improved latency and surgical field colour, reduced illumination, and ease of utilising iOCT,” Dr Talcott said.
Although the cases were not randomly assigned to the microscope group—surgeons chose whether to use the conventional or digitally enabled system—the two surgical groups were optimally matched for surgeon and preoperative diagnosis. Data on the characteristics of the conventional microscope-integrated iOCT and digitally enabled iOCT groups showed they were similar with respect to mean patient age (about 65 years for both), most common surgical indications (epiretinal membrane, 35% and 33%, respectively; retinal detachment, 21%, both groups; macular hole, 19% and 20%, respectively), and proportion of cases performed with 23-gauge instrumentation (71% and 67%, respectively).
At the end of each case, surgeons completed a standardised questionnaire designed to obtain information on surgical field visualisation along with impact of iOCT on surgical decisionmaking and surgeons’ perceptions on iOCT utility and ergonomics. The data showed they used surgical field-based iOCT visualisation in 88% of cases performed using the digitally enabled iOCT but only 7.2% of cases performed with the conventional iOCT. Looking at the converse situation, the surgeon looked away from the microscope or the 3D monitor onto the accessory screen in only 12% of cases using the digitally enabled iOCT but in 93% of those performed with the conventional iOCT, Dr Talcott reported.
Safety of using iOCT was good with both platforms—there were no intraoperative complications attributed to it, and the rate of postoperative complications was similar in the two groups. However, the endoillumination level was significantly lower using the digitally enabled system compared to the conventional iOCT (33.4% versus 37.2%, respectively).
ERGONOMIC ADVANTAGES
Ergonomics ratings also showed significant differences favouring the digitally enabled system. In cases performed with the conventional system, 22% were notable for clinically significant back discomfort and 20% for clinically significant headache. The rates for these complaints using the digitally enabled iOCT were 7% and 5%, respectively. The rate of clinically significant neck discomfort was also higher using the conventional iOCT than for the digitally enabled system (4% versus 1%, respectively), although the difference was not statistically significant.
Questions pertaining to iOCT utility showed both the conventional and digitally enabled systems were perceived to have added valuable information in the majority of cases (53% and 60%, respectively). Both the conventional and digitally enabled iOCT systems also impacted surgical decision-making in a sizeable proportion of cases (16% and 21%, respectively).
Other surgeons’ ratings of their intraoperative experience showed a strong preference (83%) for static iOCT acquisition versus real-time acquisition, regardless of the system used. There were no significant differences between the two systems in the percentages of “excellent” ratings given for quality of the widefield view and quality of the macular view. Average macular peel time was also similar in the two groups.
Dr Talcott presented at ARVO 2022 in Denver, Colorado, US. Katherine Talcott MD is a vitreoretinal surgeon practicing at the Cleveland Clinic, Ohio, US. talcotk@ccf.org
Latest Articles
Towards a Unified IOL Classification
The new IOL functional classification needs a strong and unified effort from surgeons, societies, and industry.
Organising for Success
Professional and personal goals drive practice ownership and operational choices.
Update on Astigmatism Analysis
Is Frugal Innovation Possible in Ophthalmology?
Improving access through financially and environmentally sustainable innovation.
iNovation Innovators Den Boosts Eye Care Pioneers
New ideas and industry, colleague, and funding contacts among the benefits.
José Güell: Trends in Cornea Treatment
Endothelial damage, cellular treatments, human tissue, and infections are key concerns on the horizon.
Making IOLs a More Personal Choice
Surgeons may prefer some IOLs for their patients, but what about for themselves?
Need to Know: Higher-Order Aberrations and Polynomials
This first instalment in a tutorial series will discuss more on the measurement and clinical implications of HOAs.
Never Go In Blind
Novel ophthalmic block simulator promises higher rates of confidence and competence in trainees.